Content covered in this post
- What is osteoarthritis (arthrosis)?
- Which joints are most commonly affected
- Most common symptoms
- Is osteoarthritis inflammation or “wear and tear”?
- Main causes and risk factors
- Osteoarthritis vs rheumatoid arthritis: key differences
- How osteoarthritis is diagnosed
- Most commonly requested tests
- Treatment: what actually helps
- Physical therapy and exercise for osteoarthritis
- Medications for pain and inflammation
- Joint injections and local treatments
- Do supplements like glucosamine work?
- When surgery may be necessary
- Can osteoarthritis be cured?
- Myths and facts
- Quick FAQ
- Important notice (health disclaimer)
- References and further reading
What is osteoarthritis (arthrosis)?
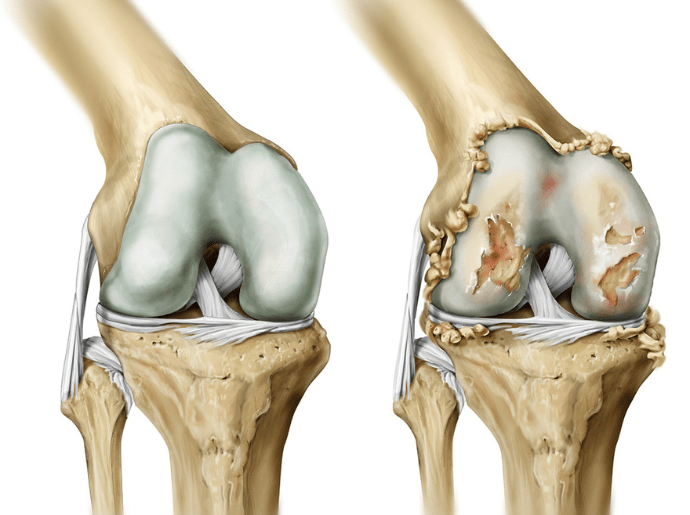
Osteoarthritis, also called arthrosis, is a chronic joint condition caused by the progressive breakdown of cartilage, the smooth tissue that covers the ends of bones and allows joints to move with minimal friction.
Cartilage works like a cushion and shock absorber. When it wears down, the joint becomes less stable and movement can become painful. Over time, the body may also develop bony growths (osteophytes), further contributing to stiffness and discomfort.
Osteoarthritis is the most common form of arthritis worldwide and becomes more frequent with age, although it can also occur earlier in people with specific risk factors.
Which joints are most commonly affected?
Osteoarthritis can affect almost any joint, but it is especially common in:
- knees
- hips
- spine (neck and lower back)
- hands (fingers and the base of the thumb)
- shoulders
Symptoms and functional limitations depend greatly on the affected joint.
Most common symptoms
Osteoarthritis symptoms typically develop gradually and worsen over time.
The most common symptoms include:
- joint pain, especially with activity
- stiffness after resting or waking up
- reduced range of motion
- joint cracking or grinding sensation (crepitus)
- mild swelling in some cases
- deformities in advanced stages (especially in the hands)
📌 A classic feature is that pain often worsens with movement and improves with rest.
Is osteoarthritis inflammation or “wear and tear”?
Osteoarthritis is primarily considered a degenerative condition, often described as a “wear and tear” disease.
However, this does not mean inflammation is absent. Many people experience episodes of inflammation within the joint, which can lead to flare-ups with swelling and increased pain.
In simple terms:
- osteoarthritis is mostly degenerative
- but inflammation can occur, especially during flare-ups
Main causes and risk factors
Osteoarthritis does not have a single cause. It usually results from a combination of mechanical, genetic, and metabolic factors.
Key risk factors include:
Age
Cartilage becomes less resilient over time, making osteoarthritis more common as people get older.
Excess weight
Extra body weight increases pressure on weight-bearing joints like the knees and hips.
Joint injuries
Previous injuries, fractures, or ligament tears can lead to earlier osteoarthritis.
Repetitive strain
Occupations or sports that overload specific joints may contribute.
Genetics
Family history plays an important role, especially in hand osteoarthritis.
Joint misalignment
Structural problems, such as bow legs or knock knees, can accelerate cartilage damage.
Osteoarthritis vs rheumatoid arthritis: key differences
Osteoarthritis and rheumatoid arthritis are often confused because both affect the joints, but they are very different conditions.
Osteoarthritis is primarily a degenerative disease caused by gradual cartilage breakdown. It is strongly associated with aging, mechanical stress, obesity, previous injuries, and genetics. It commonly affects the knees, hips, spine, and hands.
Rheumatoid arthritis, on the other hand, is an autoimmune disease. The immune system attacks the joints, causing chronic inflammation, swelling, and pain. It often causes prolonged morning stiffness and can affect multiple joints symmetrically. Rheumatoid arthritis may also involve other organs and cause fatigue and systemic symptoms.
In short:
- Osteoarthritis = degeneration and cartilage wear
- Rheumatoid arthritis = autoimmune inflammation and systemic disease
How osteoarthritis is diagnosed
Diagnosis is mainly based on:
- symptom history (type of pain and progression)
- physical examination (joint mobility, tenderness, deformities)
- imaging tests when necessary
In most cases, osteoarthritis diagnosis is straightforward.
Most commonly requested tests
Common tests include:
X-ray
The most frequently used test. It may show:
- joint space narrowing
- osteophytes (bone spurs)
- bone remodeling changes
MRI
MRI is not always needed, but it may be useful to evaluate:
- cartilage damage
- meniscus injuries
- ligaments
- early-stage changes
Blood tests
Blood tests do not diagnose osteoarthritis, but they may help rule out inflammatory arthritis, infections, or autoimmune diseases.
Treatment: what actually helps
Osteoarthritis treatment aims to reduce pain, preserve function, and improve quality of life.
The most effective approaches include:
- regular exercise and strengthening
- physical therapy
- weight loss (when appropriate)
- lifestyle adjustments
- pain control medications when needed
📌 Treatment should always be personalized based on the joint involved and severity of symptoms.
Physical therapy and exercise for osteoarthritis
Physical therapy is one of the most important parts of osteoarthritis treatment.
It helps by:
- strengthening muscles that support the joint
- improving flexibility and range of motion
- reducing stiffness and pain
- improving balance and reducing fall risk
Recommended activities often include:
- low-impact walking
- swimming and water aerobics
- cycling
- strength training under supervision
⚠️ High-impact activities may worsen symptoms in advanced cases, especially during flare-ups.
Medications for pain and inflammation
Common medications include:
- acetaminophen/paracetamol
- non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen
- topical anti-inflammatory creams or gels
- short-term muscle relaxants in selected cases
⚠️ NSAIDs should be used carefully, especially in people with stomach ulcers, kidney disease, high blood pressure, or cardiovascular risk.
Joint injections and local treatments
Some patients benefit from injections, depending on symptoms and joint involvement.
Corticosteroid injections
May reduce inflammation and pain temporarily.
Hyaluronic acid injections
May improve joint lubrication in selected patients, especially knee osteoarthritis.
PRP (platelet-rich plasma)
PRP is sometimes used, but evidence is mixed and results vary.
These procedures should always be guided by a specialist.
Do supplements like glucosamine work?
Glucosamine and chondroitin are widely used supplements, but scientific evidence remains inconsistent.
Some people report mild symptom improvement, but:
- benefits are not guaranteed
- effects are usually modest
- there is no strong evidence that they rebuild cartilage
Discuss supplement use with a healthcare professional, especially if you take other medications.
When surgery may be necessary
Surgery may be considered when:
- pain becomes severe and persistent
- mobility and daily function are significantly reduced
- conservative treatment fails
- deformities become advanced
Surgical options may include:
- joint-preserving procedures in selected cases
- joint replacement surgery (hip or knee replacement)
Joint replacement can significantly improve pain and quality of life in advanced osteoarthritis.
Can osteoarthritis be cured?
Osteoarthritis is a chronic condition and is not usually curable.
However, it can often be successfully managed. Many people can reduce pain, improve mobility, and slow progression with proper treatment and lifestyle changes.
Early intervention is key.
Myths and facts
“Osteoarthritis is just normal aging and nothing can be done.”
Myth. Effective treatment exists and can greatly improve function.
“Exercise makes osteoarthritis worse.”
Myth. Proper exercise is one of the best treatments.
“Weight loss can significantly improve knee osteoarthritis.”
Fact. Reducing weight lowers mechanical stress on joints.
“Bone spurs always cause pain.”
Myth. Many people have osteophytes without symptoms.
Quick FAQ
Can young people get osteoarthritis?
Yes, especially after joint injuries, obesity, or genetic predisposition.
Should I avoid walking if I have osteoarthritis?
Not necessarily. Low-impact walking is often beneficial.
Does osteoarthritis cause swelling?
It can, especially during flare-ups.
Can osteoarthritis worsen quickly?
It usually progresses slowly, but progression can accelerate with joint overload and lack of treatment.
When should I see a doctor?
If joint pain is persistent, limits daily activities, or progressively worsens.
Important notice (health disclaimer)
This content is for educational purposes only and does not replace professional medical advice. Persistent joint pain, significant stiffness, swelling, deformity, or difficulty walking should be evaluated by a healthcare professional for proper diagnosis and treatment.
References and further reading
World Health Organization (WHO). Musculoskeletal conditions overview.
Centers for Disease Control and Prevention (CDC). Osteoarthritis information.
National Health Service (NHS). Osteoarthritis: symptoms and treatment.
Mayo Clinic. Osteoarthritis: symptoms and causes.
American College of Rheumatology (ACR). Osteoarthritis guidance and resources.