What this post covers
- What tinea versicolor is
- Why this fungal infection is so common
- Is tinea versicolor contagious?
- Common symptoms and how to recognize it
- Where it usually appears on the body
- Tinea versicolor vs. vitiligo: how to tell the difference
- Tests used for diagnosis
- Treatment: shampoos, creams, and oral antifungals
- How long it takes for skin color to return to normal
- Why tinea versicolor often comes back
- How to prevent recurrence
- When to see a dermatologist
- Myths and facts
- Quick FAQ
- Medical disclaimer
- References and recommended reading
What is tinea versicolor?
Tinea versicolor, also called pityriasis versicolor, is a common superficial fungal infection of the skin.
It is caused by Malassezia, a type of yeast that naturally lives on the skin. In some people, this yeast overgrows and interferes with normal pigmentation, leading to patches that may appear:
- lighter than the surrounding skin
- darker than the surrounding skin
- slightly pink or reddish in some cases
📌 Despite the name, this condition is not always “white.” The color varies depending on skin tone and sun exposure.
Why is this fungal infection so common?
Malassezia is part of the skin’s normal microbiome, especially in oily areas. Tinea versicolor occurs when conditions favor yeast overgrowth.
Common triggers include:
- hot and humid weather
- excessive sweating
- oily skin
- wearing tight or non-breathable clothing
- frequent physical activity
- use of oily skincare products
- weakened immune function (in some cases)
📌 This is why tinea versicolor often becomes more noticeable during warmer seasons.
Is tinea versicolor contagious?
Tinea versicolor is not usually considered contagious in the typical sense.
Since Malassezia normally lives on many people’s skin, the condition is more related to an imbalance that allows overgrowth rather than direct transmission from another person.
📌 Most cases are linked to individual predisposition and environmental factors.
Common symptoms and how to recognize it
Tinea versicolor typically causes patches of skin discoloration with subtle scaling.
Common signs and symptoms
- lighter or darker patches on the skin
- fine scaling (a powdery texture when rubbing the skin)
- mild itching in some cases
- patches becoming more noticeable after sun exposure
📌 Fine scaling is one of the most helpful clues for diagnosis.
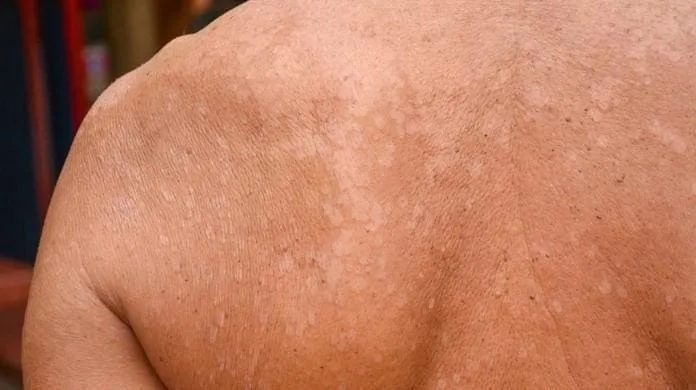
Where does it usually appear?
Tinea versicolor most often affects the upper body, especially areas with higher oil production.
Common locations include:
- upper back
- chest
- shoulders
- upper arms
- neck
- upper abdomen
It is less common on the hands and lower legs.
Tinea versicolor vs. vitiligo: how to tell the difference
Many people confuse tinea versicolor with vitiligo, but they are very different conditions.
Tinea versicolor
- often has fine scaling
- may be lighter, darker, or slightly pink
- usually affects the trunk and shoulders
- improves with antifungal treatment
- skin color may take time to normalize after treatment
Vitiligo
- sharply defined white patches
- no scaling
- often affects face, hands, and areas around the eyes and mouth
- is autoimmune, not fungal
- does not respond to antifungal medication
📌 If there is any doubt, a dermatologist can usually confirm the diagnosis quickly.
Tests used for diagnosis
Diagnosis is often clinical, based on the appearance of the patches.
When needed, doctors may use:
Wood’s lamp examination
A painless UV light test that helps highlight areas of altered pigmentation.
Skin scraping (microscopy)
A small sample of skin is examined under a microscope to confirm the presence of yeast.
📌 This test is quick and painless.
Treatment: shampoos, creams, and oral antifungals
Treatment is usually effective, but it must be used correctly.
Topical treatment (most common)
This may include:
- antifungal shampoos (ketoconazole or selenium sulfide)
- antifungal lotions
- antifungal creams
Shampoos are often applied to the affected skin (not just the scalp), left on for several minutes, and then rinsed off.
📌 Treatment is typically recommended daily for several days or weeks, depending on severity.
Oral antifungal treatment (for extensive or recurrent cases)
If the infection is widespread or frequently recurring, a doctor may prescribe oral antifungal medications such as:
- itraconazole
- fluconazole
⚠️ Oral antifungals should only be used under medical supervision, as they may cause side effects and interact with other medications.
How long does it take for skin color to return to normal?
This is one of the most common concerns.
Even after the yeast is eliminated, skin pigmentation may take weeks or even months to fully return to normal.
This delay happens because:
- pigment-producing cells need time to recover
- sun exposure may have created contrast between affected and unaffected skin
📌 Persistent discoloration does not necessarily mean the infection is still active.
Why does tinea versicolor often come back?
Tinea versicolor has a high recurrence rate, especially in individuals who are prone to it.
Recurrence happens because:
- Malassezia remains part of the normal skin flora
- heat and sweating promote yeast growth
- oily skin increases susceptibility
- humid climates create ideal conditions
📌 Many people experience repeated flare-ups during warmer months.
How to prevent recurrence
Prevention is especially important for those who have frequent episodes.
Practical prevention tips
- avoid staying in sweaty clothing for long periods
- shower soon after workouts
- wear breathable clothing
- avoid heavy oily lotions on the trunk
- keep skin dry in hot weather
- use antifungal shampoo preventively if recommended by a healthcare professional
📌 Some dermatologists recommend weekly or monthly use of antifungal shampoo during high-risk seasons.
When to see a dermatologist
You should seek medical evaluation if:
- patches spread quickly
- itching becomes significant
- symptoms do not improve with treatment
- the condition returns frequently
- you are unsure if it is vitiligo or another skin condition
- you have immune system problems or take immunosuppressive medications
📌 Proper diagnosis is important, since many other skin conditions can cause similar discoloration.
Myths and facts
“Tinea versicolor is caused by poor hygiene.”
Myth. It is mainly related to yeast overgrowth, not cleanliness.
“It spreads easily from person to person.”
Mostly a myth. The yeast is commonly present on healthy skin.
“The patches disappear immediately after treatment.”
Myth. Pigment recovery can take weeks or months.
“Sun exposure helps cure it.”
Myth. Sun exposure often makes the contrast more noticeable.
“Tinea versicolor often comes back.”
Fact. Recurrence is common.
Quick FAQ
Can tinea versicolor be cured?
Yes. Treatment can eliminate the overgrowth, but recurrence is common.
Is tinea versicolor dangerous?
No. It is usually harmless, but it can be persistent and cosmetically distressing.
Can I use antifungal shampoo on my body?
Yes. This is one of the most common treatment approaches.
How long does treatment take?
Usually days to weeks, depending on severity and the medication used.
Should I use steroid creams?
Not recommended. Steroids can worsen fungal infections or mask symptoms.
Which specialist should I see?
A dermatologist is the best specialist for diagnosis and management.
Medical disclaimer
This content is for educational purposes only and does not replace medical advice. Skin discoloration can have multiple causes. If the diagnosis is uncertain, symptoms recur frequently, or treatment does not work, seek evaluation from a qualified healthcare professional.
References and recommended reading
- American Academy of Dermatology (AAD). Tinea versicolor: overview and treatment.
- Mayo Clinic. Tinea versicolor: symptoms and causes.
- National Health Service (NHS). Pityriasis versicolor guidance.
- British Association of Dermatologists (BAD). Patient information: pityriasis versicolor.
- UpToDate. Tinea versicolor: clinical features and management.