Content covered in this post
What is Polycystic Ovary Syndrome (PCOS)?
Is PCOS an endocrine disorder or a reproductive condition?
Main symptoms of PCOS
What causes PCOS
Common risk factors
PCOS and insulin resistance: what is the connection?
How PCOS is diagnosed
Most common tests and exams
Possible complications
PCOS and fertility: can you get pregnant?
Treatment: lifestyle changes
Medical treatment options
When birth control may be recommended
Metformin and PCOS
Treatments for acne and excess hair growth
Myths and facts
Quick FAQ
Important notice (health disclaimer)
References and further reading
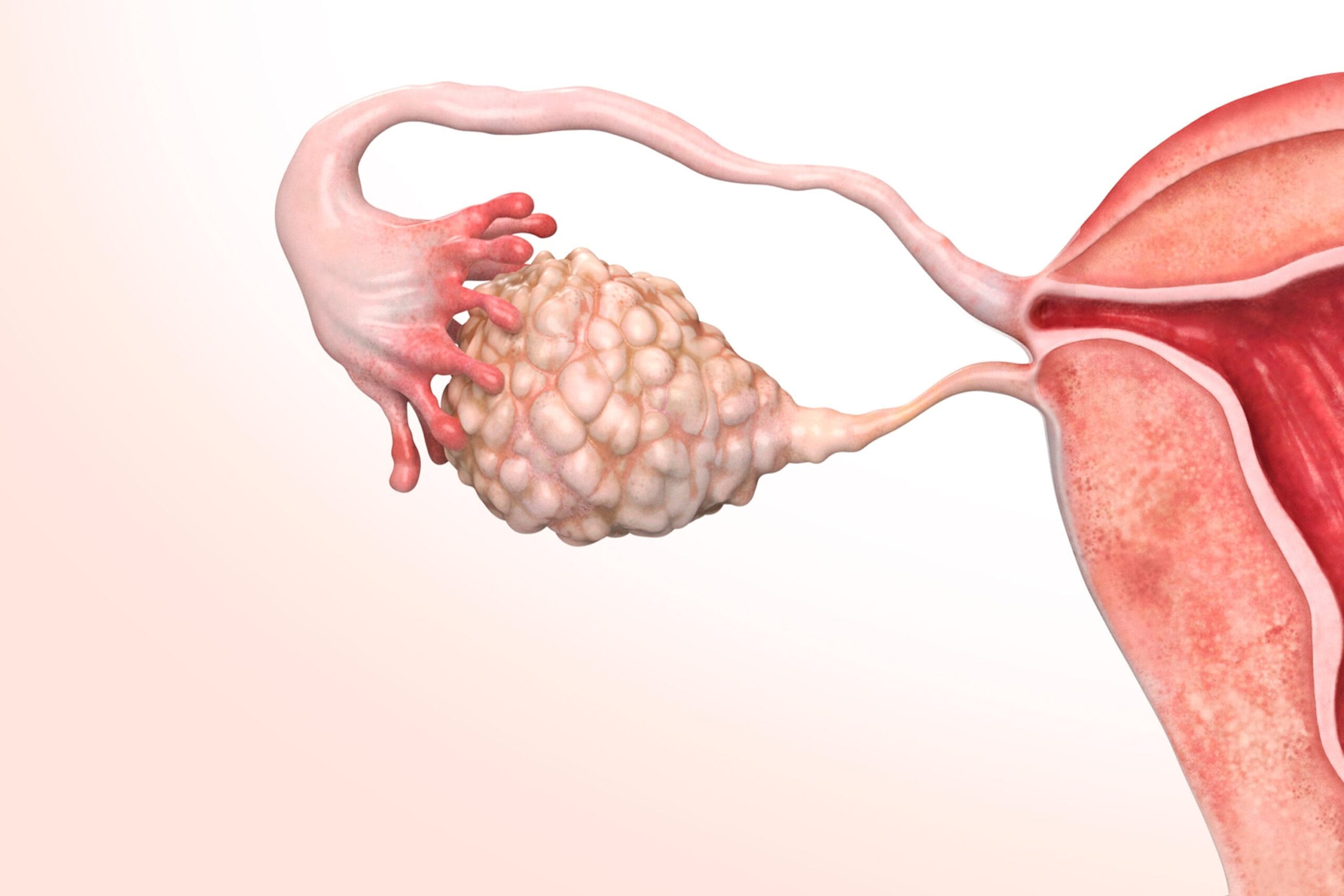
What is Polycystic Ovary Syndrome (PCOS)?
Polycystic Ovary Syndrome (PCOS) is a common condition affecting people with ovaries, especially during reproductive age. It is mainly associated with hormonal imbalance, particularly involving increased levels of androgens (often called “male hormones,” though they are naturally present in all sexes).
Despite its name, PCOS does not necessarily mean there are true “cysts” in the ovaries. What is often seen on ultrasound are multiple small follicles, which reflect changes in normal ovulation.
PCOS can cause menstrual irregularities, skin and hair-related symptoms, and significant metabolic effects.
Is PCOS an endocrine disorder or a reproductive condition?
This is a very common question.
PCOS affects the reproductive system, as it can interfere with ovulation, menstrual cycles, and fertility. However, its underlying mechanisms are largely hormonal and metabolic, which is why PCOS is widely considered an endocrine disorder.
Many people with PCOS also experience:
elevated androgen levels
insulin resistance
weight gain or difficulty losing weight
increased risk of type 2 diabetes
For this reason, PCOS is often managed by both gynecologists and endocrinologists.
Main symptoms of PCOS
Symptoms can vary significantly. Some people have mild symptoms, while others experience more severe hormonal and metabolic changes.
The most common symptoms include:
Menstrual changes
irregular periods
long cycles (more than 35 days)
missed periods for months
unpredictable bleeding patterns
Signs of high androgen levels
persistent acne (especially jawline and lower face)
excess hair growth on the face, chest, or abdomen (hirsutism)
scalp hair thinning or hair loss
Metabolic symptoms
weight gain, especially around the abdomen
difficulty losing weight
increased appetite and fatigue
Other possible signs
oily skin
darkened patches of skin in body folds (acanthosis nigricans)
emotional distress related to self-image and chronic symptoms
What causes PCOS?
PCOS does not have a single cause. It is considered a multifactorial condition involving genetic and hormonal factors.
The main mechanisms include:
hormonal imbalance with increased androgen production
irregular or absent ovulation
insulin resistance, which can stimulate the ovaries to produce more androgens
This creates a cycle that may worsen symptoms over time if not managed.
Common risk factors
Certain factors may increase the risk of PCOS or worsen symptoms:
family history of PCOS
overweight or obesity
insulin resistance
sedentary lifestyle
family history of type 2 diabetes
hormonal irregularities starting in adolescence
It is important to note that PCOS can also occur in people with normal weight.
PCOS and insulin resistance: what is the connection?
Insulin resistance is one of the most important metabolic features of PCOS.
When the body becomes less responsive to insulin, the pancreas produces more insulin to compensate. High insulin levels can stimulate the ovaries to produce more androgens, worsening symptoms such as acne, excess hair growth, and irregular periods.
Insulin resistance also increases the risk of:
prediabetes
type 2 diabetes
abnormal cholesterol levels
fatty liver disease
That is why PCOS should not be seen only as a reproductive condition, but also as a metabolic health issue.
How PCOS is diagnosed
PCOS is diagnosed through clinical evaluation and laboratory testing.
The most widely used diagnostic approach is the Rotterdam Criteria, which requires at least two of the following threefeatures:
irregular or absent ovulation (often reflected by irregular periods)
clinical or laboratory signs of high androgen levels
polycystic ovarian appearance on ultrasound
Other conditions that can mimic PCOS must also be ruled out before confirming the diagnosis.
Most common tests and exams
Testing varies depending on symptoms, but commonly includes:
pelvic ultrasound
total and free testosterone
SHBG (sex hormone-binding globulin)
LH and FSH
prolactin
TSH (thyroid function test)
fasting glucose and HbA1c
insulin levels (when appropriate)
lipid profile (cholesterol and triglycerides)
These tests help confirm the diagnosis and assess metabolic risks.
Possible complications
Without proper management, PCOS may increase the risk of several long-term health issues, including:
infertility due to irregular ovulation
type 2 diabetes
high blood pressure and cardiovascular risk
dyslipidemia (high cholesterol)
fatty liver disease
sleep apnea (in some cases)
anxiety and depression
endometrial hyperplasia (thickening of the uterine lining)
increased risk of endometrial cancer in people with prolonged absence of periods
The increased risk of endometrial problems occurs because irregular ovulation can lead to prolonged estrogen exposure without the balancing effect of progesterone.
PCOS and fertility: can you get pregnant?
Yes. Most people with PCOS can become pregnant, although some may have difficulty due to irregular ovulation.
With proper medical support, fertility can often improve through:
weight management (when relevant)
metabolic control
ovulation-inducing medications when needed
Many people conceive naturally once hormonal balance improves.
Treatment: lifestyle changes
Lifestyle changes are often the foundation of PCOS treatment, especially when insulin resistance or excess weight is present.
The most effective strategies include:
balanced diet with fewer ultra-processed foods
regular physical activity
improved sleep habits
stress management
weight loss when appropriate (even 5–10% can significantly improve symptoms)
Lifestyle improvements may help regulate periods, reduce insulin resistance, improve fertility, and reduce acne severity.
Medical treatment options
Treatment depends on individual goals, such as symptom control, cycle regulation, skin improvement, or fertility.
Common medical options include:
hormonal birth control (to regulate cycles and reduce androgen effects)
metformin (especially in insulin resistance or prediabetes)
ovulation induction medications for those trying to conceive
anti-androgen medications in selected cases (with careful supervision)
Treatment should always be individualized.
When birth control may be recommended
Hormonal birth control is often recommended to:
regulate menstrual cycles
reduce acne and oily skin
decrease excess hair growth
protect the endometrium from long-term irregular bleeding risks
It does not “cure” PCOS, but it can effectively control symptoms and reduce complications.
Metformin and PCOS
Metformin is a medication that improves insulin sensitivity.
It may be recommended for people with PCOS who have:
insulin resistance
prediabetes
obesity
very irregular cycles
In some cases, metformin may help regulate menstrual cycles and support weight management when combined with lifestyle changes.
Treatments for acne and excess hair growth
In addition to hormonal control, other treatments may help:
For acne:
topical dermatologic treatments
oral antibiotics in certain cases
isotretinoin for severe acne (under medical supervision)
For excess hair growth:
laser hair removal
cosmetic treatments
anti-androgen medications (only with medical guidance)
Improvement is usually gradual and may take several months.
Myths and facts
“PCOS means you have cysts on your ovaries.”
Myth. PCOS is primarily a hormonal and metabolic syndrome, and cysts are not always present.
“If you have PCOS, you can’t get pregnant.”
Myth. Many people with PCOS conceive naturally or with treatment.
“Only overweight people get PCOS.”
Myth. PCOS can occur in people of any weight.
“PCOS increases diabetes risk.”
Fact. Insulin resistance is common in PCOS and increases the risk of type 2 diabetes.
“Lifestyle changes make a real difference.”
Fact. For many people, lifestyle changes are one of the most effective treatments.
Quick FAQ
Is PCOS curable?
There is no definitive cure, but symptoms can be well controlled with proper treatment.
Can PCOS cause missed or irregular periods?
Yes. Irregular menstruation is one of the most common signs.
Do I need to take birth control forever?
Not necessarily. Treatment depends on symptoms and individual goals.
Can PCOS cause hair loss?
Yes. Increased androgen levels may lead to scalp hair thinning in some individuals.
Can ultrasound confirm PCOS on its own?
No. Ultrasound helps, but diagnosis also depends on symptoms and hormone testing.
Important notice (health disclaimer)
This content is for educational purposes only and does not replace professional medical advice. Persistent irregular periods, severe acne, excess hair growth, hair loss, or fertility concerns should be evaluated by a healthcare professional for accurate diagnosis and personalized treatment.
References and further reading
American College of Obstetricians and Gynecologists (ACOG). Polycystic Ovary Syndrome (PCOS).
Endocrine Society. Clinical Practice Guidelines for PCOS.
Centers for Disease Control and Prevention (CDC). PCOS information and resources.
World Health Organization (WHO). Reproductive health and endocrine disorders resources.