Topics covered in this post
What alopecia is
The most common types and how to tell them apart
Red flags and systemic causes
Diagnosis: what happens at the visit
Treatments by alopecia type
Realistic expectations and time to see results
Myths and facts about hair loss
Quick FAQ
Important notice (health disclaimer)
How VirtualCare can help
References and recommended reading
What alopecia is
Alopecia is the medical term for hair loss or hair thinning. It can be temporary or permanent, inflammatory or non-inflammatory, and it may affect the scalp, eyebrows, eyelashes, and body hair. Identifying the type of alopecia is the most important step, because treatment depends on the cause.
The most common types and how to tell them apart
Androgenetic alopecia
Genetic and hormonal hair loss. In men, hairline recession and thinning at the vertex. In women, diffuse thinning over the crown with a preserved frontal hairline. Slow progression with follicle miniaturization.
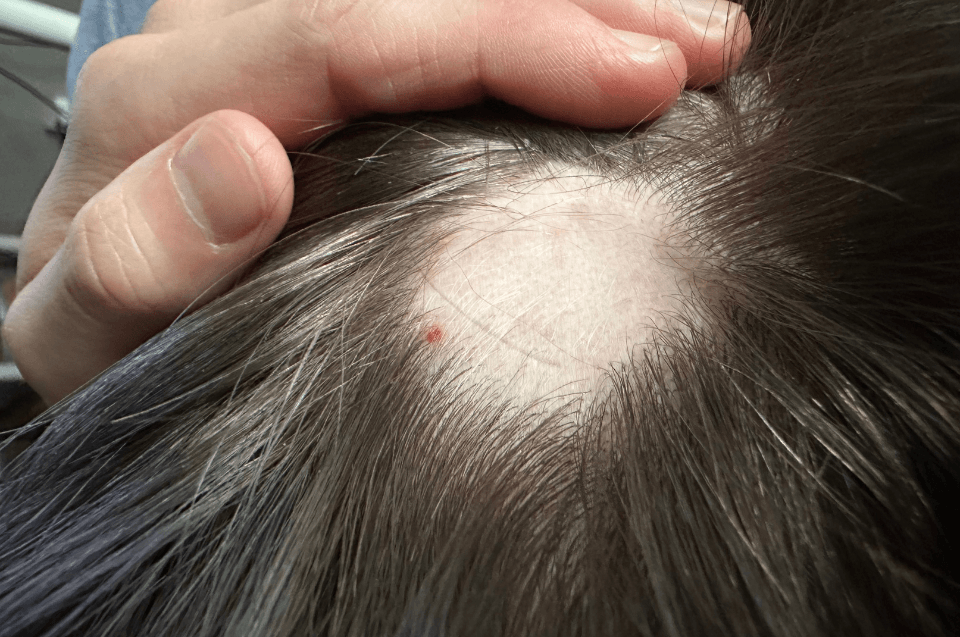
Alopecia areata
Round, smooth, hairless patches that can merge. Eyebrows and eyelashes may be involved. In some cases it presents diffusely. It is autoimmune and unpredictable, with phases of shedding and regrowth.
Telogen effluvium
Diffuse shedding, usually 2 to 3 months after a trigger such as fever, infection, childbirth, surgery, very restrictive diets, major stress, or iron deficiency. More hair comes out when washing or combing, without sharply demarcated bald patches.
Scarring alopecias
Inflammation permanently destroys follicles. Examples: lichen planopilaris, frontal fibrosing alopecia, CCCA. Look for areas with loss of follicular openings, fine scale, pain or burning. They need prompt diagnosis and treatment to prevent permanent loss.
Traction alopecia
Tight hairstyles, braids, or repeated chemical treatments. Begins along the frontal hairline and areas under greater traction. Reversible early on, but can scar if it continues for a long time.
Tinea capitis
Fungal infection, more common in children. Patches with scale, broken hairs, and sometimes enlarged lymph nodes. Requires oral antifungals.
Red flags and systemic causes
Some conditions worsen or trigger hair loss: iron deficiency, vitamin D deficiency (associated with alopecia areataand usually not a standalone cause), thyroid dysfunction, certain medications, nutritional disorders, lupus and other autoimmune diseases. When clinically suspected, it is reasonable to check 25-OH vitamin D and correct deficiency as an adjunct to dermatologic treatment, not as a substitute. Warning signs include shedding with intense itching, scalp pain, persistent redness, heavy scaling, or loss of eyebrows and eyelashes.
Diagnosis: what happens at the visit
The dermatologist reviews medical history, hair-care habits, and overall health. On exam, they assess the thinning pattern, perform a hair pull test, and use trichoscopy to examine follicular openings and hair shafts. Blood work may include ferritin and iron, TSH, and other tests based on suspicion. For scarring alopecias or unclear cases, a scalp biopsy may be needed.
Treatments by alopecia type
Androgenetic alopecia
Minoxidil 5 percent topical foam or solution, used daily. Low-dose oral minoxidil is an option in selected cases with monitoring.
Finasteride for men, with discussion of sexual side effects and the need for ongoing use. Dutasteride is off label in some settings.
Women: antiandrogens such as spironolactone may help. Finasteride and dutasteride require discussion of teratogenicity and contraception.
Adjuncts: microneedling, low-level laser therapy, and PRP (platelet-rich plasma) have variable results.
Hair transplantation is an option when there is a suitable donor area and stable disease. It complements, rather than replaces, medical therapy.
Alopecia areata
Intralesional corticosteroids for active patches and potent topical steroids for more extensive areas.
Contact immunotherapy in specialized centers.
JAK inhibitors for moderate to severe disease, with risk evaluation and monitoring.
Bimatoprost topical can be considered for eyebrows and eyelashes.
Telogen effluvium
Identify and treat the trigger.
Correct iron deficiency when present.
Educate about the recovery timeline: regrowth usually begins in 3 to 6 months and full volume may take 9 to 12 months.
Scarring alopecias
Control inflammation with topical or intralesional corticosteroids, anti-inflammatory antibiotics such as doxycycline, and in selected cases hydroxychloroquine or other immunomodulators.
Transplantation only after the disease is inactive for a long period and after careful evaluation.
Traction alopecia
Change hairstyles, reduce traction and chemical exposure. Treat associated inflammation when present. The earlier the change, the higher the chance of recovery.
Tinea capitis
Oral antifungals (for example, griseofulvin or terbinafine) and antifungal shampoos as adjuncts. Treat close contacts when indicated.

Realistic expectations and time to see results
Minoxidil often causes increased shedding in the first weeks, then stabilizes. Early improvement typically appears at 3 to 6 months.
Hormonal treatments and antiandrogens require continuous use with periodic review.
In areata, the course is fluctuating. Even with good response, new flares can occur.
Scarring alopecias prioritize halting progression. Areas that are already scarred do not regrow.
Myths and facts about hair loss
“Shaving makes hair thicker.” Myth. Blades do not change hair shaft diameter.
“Biotin fixes everything.” Myth. Supplements help only in documented deficiency.
“Anti-hair loss shampoos cure baldness.” Myth. They may improve scalp health but do not reverse miniaturization.
“Very restrictive diets do not matter.” Myth. They can trigger telogen effluvium.
“Shedding after COVID or childbirth is permanent.” Usually telogen effluvium, which resolves with time and proper management.
Quick FAQ
Sudden clumps of hair loss, should I worry?
Yes. Seek evaluation, especially if there is pain, intense itching, redness, or well-defined bald patches.
Is oral minoxidil safe?
It can be used at low doses with medical follow-up. Screen for contraindications and monitor for edema and tachycardia.
Does finasteride always cause sexual side effects?
Most people tolerate it well. Side effects are uncommon, but they should be discussed and monitored.
Does a hair transplant replace medication?
No. Even after transplantation, many people continue medical therapy to preserve native hair.
Important notice (health disclaimer)
This content is educational and does not replace medical care. Hair loss has many causes, and treatment should be individualized after the correct diagnosis.
References and recommended reading
American Academy of Dermatology (AAD). Hair loss types and treatments, guidance for patients and clinicians.
European Dermatology Forum. Guideline on the diagnosis and treatment of alopecia areata and scarring alopecias.
British Association of Dermatologists. Guidelines for the management of androgenetic alopecia and alopecia areata.
JAMA Dermatology and The New England Journal of Medicine (NEJM). Clinical trials on therapies for alopecia areata and androgenetic alopecia, including JAK inhibitors.
Cochrane Reviews. Minoxidil and adjunctive therapies for hair loss.
International Society of Hair Restoration Surgery (ISHRS). Best practices in hair transplantation and candidate selection.