Content discussed in this post
What melanoma is
Warning signs and skin self-exam
Risk factors and when to suspect it
Types of melanoma and special locations
Diagnosis: from clinical exam to biopsy
Staging: Breslow, sentinel lymph node, and imaging
Treatment by stage
Follow-up and surveillance
Prevention and real-life photoprotection
Quick FAQ
Important notice (health disclaimer)
References and recommended reading
What melanoma is
Melanoma is a skin cancer that arises from melanocytes, the cells that produce melanin. Although less common than other skin cancers, it typically has a higher metastatic potential. Cure rates are very high when the diagnosis is made early and the lesion is removed with adequate margins. The thicker the lesion at diagnosis, the greater the risk of spread.
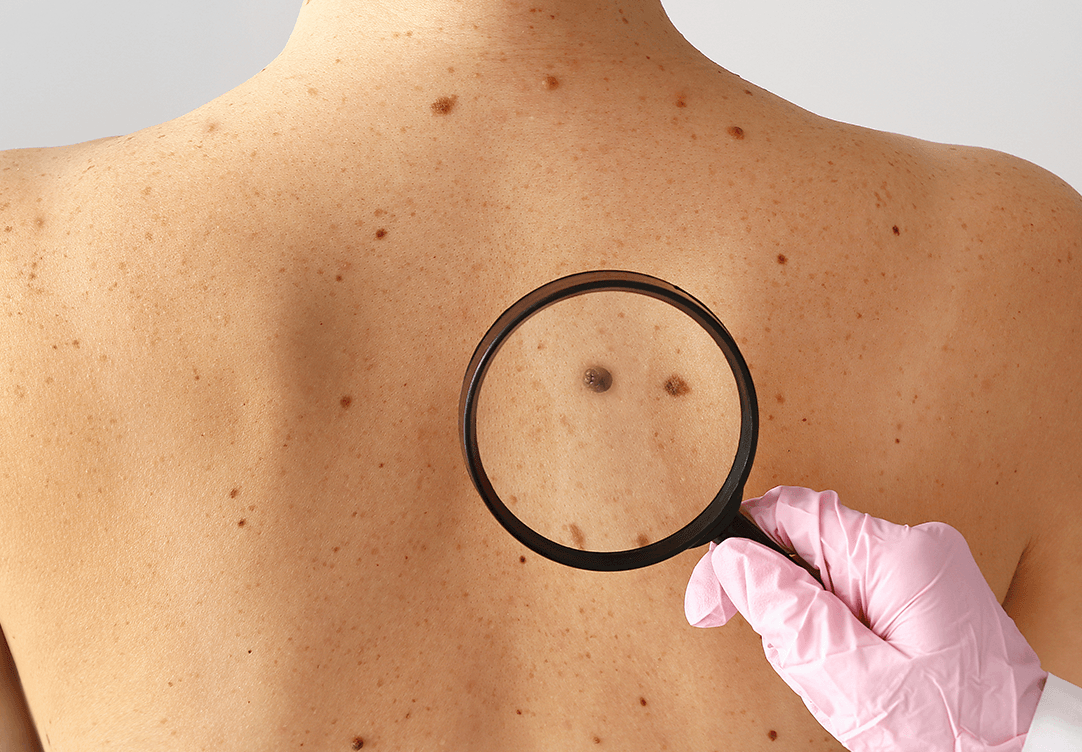
Warning signs and skin self-exam
Learning to recognize suspicious changes helps you seek care at the right time. Two simple strategies:
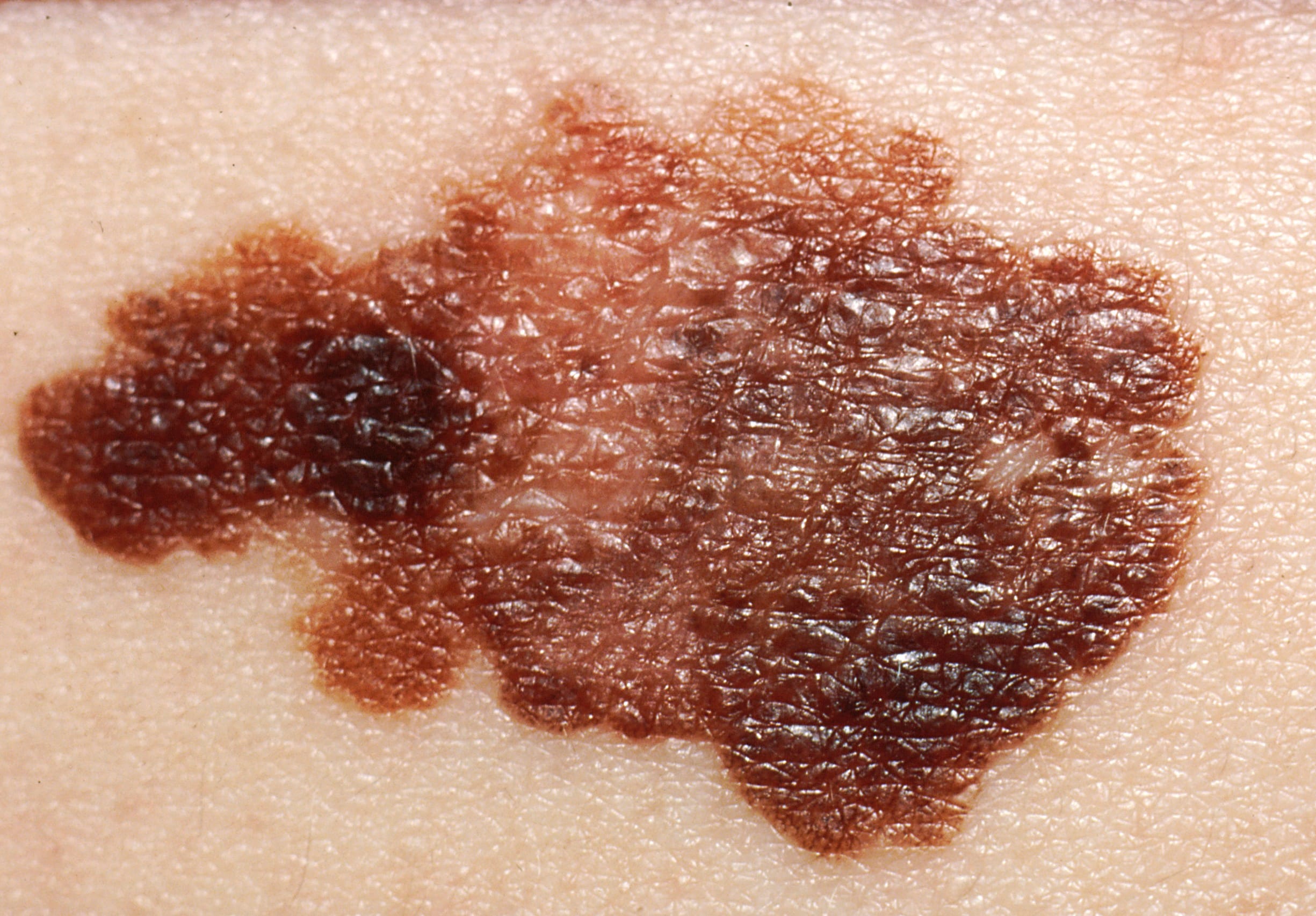
The ABCDE rule
A (Asymmetry): one half looks different from the other.
B (Border): irregular or poorly defined edges.
C (Color): multiple colors within the same lesion, such as black, brown, gray, red, white, or blue.
D (Diameter): larger than 6 mm, keeping in mind that melanomas can be smaller.
E (Evolution): any recent change in size, shape, color, elevation, bleeding, or itching.
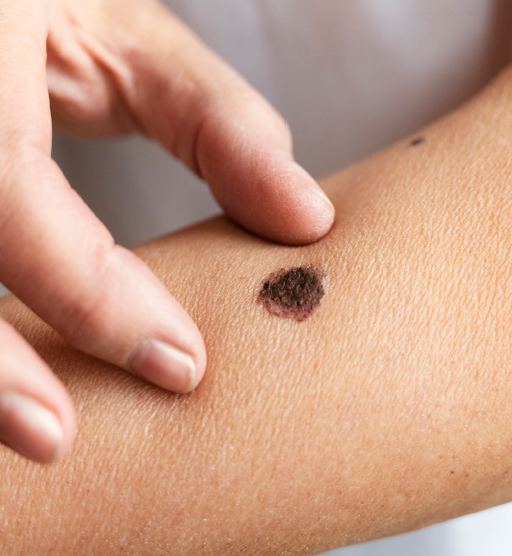
The “ugly duckling” sign
Among your moles, the one that looks different from the rest deserves evaluation, even if it is small.
Do a monthly self-exam using a mirror and, if possible, help from another person for the back and scalp. Photograph key moles to compare changes over time.
Risk factors and when to suspect it
Cumulative sun exposure, sunburns in childhood and adolescence, and use of tanning beds
Fair skin, light eyes, blond or red hair, freckles
Many nevi and the presence of atypical nevi
Personal or family history of melanoma
Immunosuppression due to disease or medications
Certain rare genetic syndromes
Pigmented lesions on the nails, such as a dark band that widens or distorts the nail, and lesions on the soles and palms also require attention. This is especially relevant in people with darker skin, in whom acral lentiginous melanomas are relatively more common.
Types of melanoma and special locations
Superficial spreading: the most common type, initially grows along the surface.
Nodular: tends to grow in depth more quickly and is often raised and dark.
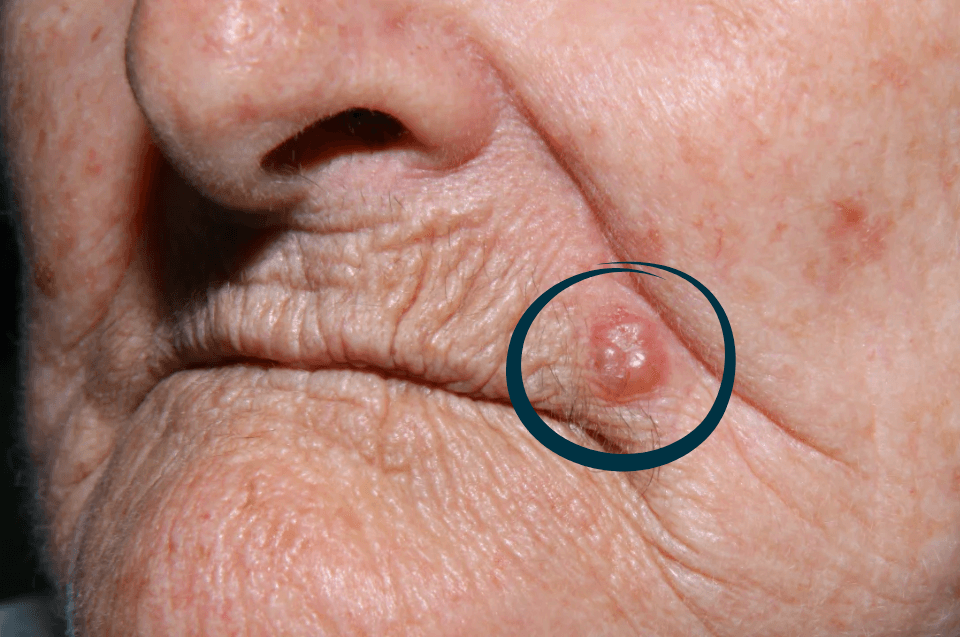
Lentigo maligna melanoma: typical of chronically sun-exposed areas in older adults.
Acral lentiginous: occurs on palms, soles, and nails, and can be overlooked.
Mucosal: rare, found on oral, nasal, genital, or anal mucosa.
Special locations require trained evaluation and often dermoscopy.
Diagnosis: from clinical exam to biopsy
Evaluation begins with a clinical exam and dermoscopy. If melanoma is suspected, an excisional biopsy of the entire lesion with a small safety margin is performed. In specific situations, an incisional biopsy may be done. The pathology report provides:
Breslow thickness in millimeters, a central prognostic factor
Presence or absence of ulceration
Mitotic rate and margins
Histologic subtype and other relevant features
These data guide staging and the treatment plan.
Staging: Breslow, sentinel lymph node, and imaging
Staging considers thickness, lymph node involvement, and distant metastases.
Lesions meeting certain Breslow cutoffs or other risk factors may indicate sentinel lymph node biopsy, a procedure that checks for tumor cells in the first draining lymph node of that region.
Imaging tests such as ultrasound, CT, and PET-CT are used when there is nodal risk, clinical suspicion, or advanced disease. The goal is precise classification to choose the most appropriate treatment.
Treatment by stage
Treatment is individualized and defined by a multidisciplinary team.
Localized disease
Surgical excision with safety margins proportional to Breslow thickness
Sentinel lymph node biopsy for staging when indicated
In select higher-risk cases, adjuvant therapy may be considered
Nodal disease or high-risk features
Lymph node surgery when appropriate
Adjuvant immunotherapy with PD-1 inhibitors, for example pembrolizumab or nivolumab, to reduce recurrence risk
For tumors with BRAF V600 mutations, targeted therapy combining BRAF and MEK inhibitors may be used in selected scenarios
Metastatic disease
Immunotherapy with anti–PD-1 alone or combined with anti–CTLA-4 is a mainstay and can provide durable responses in some patients
Targeted therapy for BRAF V600 tumors, paired with MEK inhibition, often produces rapid responses that are useful in symptomatic disease
Radiotherapy can help control symptomatic metastases, such as in the brain or bone
Decisions consider disease extent, mutations, symptoms, comorbidities, and patient preferences.
Follow-up and surveillance
After treatment, follow-up aims to detect recurrences and new melanomas and to reinforce photoprotection. Visit frequency and the need for imaging vary by initial stage. Self-exam remains important. Any new suspicious mole or changes in a surgical scar should be evaluated.
Prevention and real-life photoprotection
Avoid sunburns
Use broad-spectrum sunscreen that protects against UVA and UVB, SPF 30 or higher for daily use, reapplying every 2 hours with continuous exposure and after sweating or swimming. Apply an adequate amount, including ears, nape, and the tops of the feet
Wear UPF clothing, a wide-brimmed hat, and sunglasses
Seek shade between 10 a.m. and 4 p.m. when possible
Indoor tanning is not safe and increases melanoma risk
Teach children and adolescents about photoprotection and model the behavior at home
Quick FAQ
Is every changing mole cancer?
No. Changes should be assessed, but many are benign. The ABCDE rule and the ugly duckling sign help decide when to see a dermatologist.
Does sunscreen alone prevent melanoma?
It is one part of a protection package. Best results come from combined strategies: sunscreen, clothing, hats, shade, and planning outdoor times.
Can melanoma occur in dark skin?
Yes. It is less common but does occur, particularly on palms, soles, and nails. Everyone benefits from education on warning signs.
Can someone who had melanoma develop another one?
Yes. The risk of a second melanoma is higher than in the general population, which is why follow-up is essential.
Does pregnancy change the risk?
Moles may darken due to hormonal influence and skin stretching. Any suspicious lesion during pregnancy should be promptly evaluated, with biopsy when indicated.
Important notice (health disclaimer)
This content is educational and does not replace medical consultation. Suspicious skin lesions should be evaluated by qualified professionals. Treatment plans are individualized and defined by specialized teams.
References and recommended reading
WHO/IARC. Solar radiation and skin cancer, prevention, and photoprotection education.
American Academy of Dermatology. Guides for self-exam, ABCDE, and photoprotection.
AJCC. Melanoma staging manual, current criteria.
NCCN Guidelines. Cutaneous melanoma: diagnosis, treatment, and follow-up.
ESMO Clinical Practice Guidelines. Cutaneous melanoma, stage-based management and systemic therapies.
Cochrane Reviews. Effectiveness of sunscreen and combined photoprotection strategies.
SEER/NIH. Incidence, survival, and trend data.